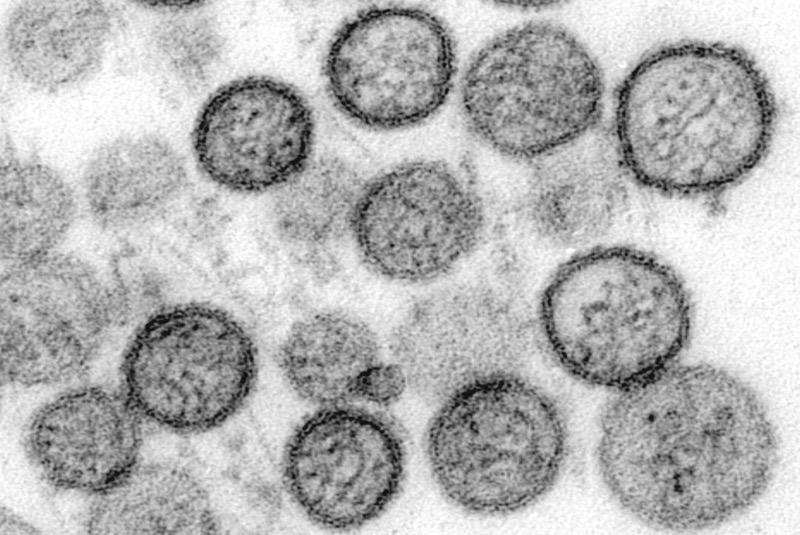
A cruise ship drifting across the Atlantic has become the latest reminder that obscure pathogens can disrupt a tightly connected world. The MV Hondius, travelling from Argentina to Cape Verde, has been linked to a cluster of hantavirus infections, with three confirmed cases, several more suspected, and at least one death. Two infected passengers were evacuated to South Africa, where officials confirmed the presence of the Andes strain, a rare variant known for its unusual capacity—albeit limited—to spread between humans. As the vessel seeks to dock in the Canary Islands, passengers have been confined to their cabins, and health authorities are racing to understand how the outbreak began and whether it can be contained.
Hantaviruses are not a single disease but a family of viruses, first identified near the Hantan River in South Korea during the Korean War. More than 20 distinct species are now recognised, most of which are carried by rodents and transmitted to humans through contact with contaminated urine, droppings or saliva. Infection typically occurs when viral particles become airborne and are inhaled, often in enclosed or poorly ventilated environments. Unlike respiratory viruses such as influenza, hantaviruses do not usually spread through casual person-to-person contact. The Andes strain, however, stands apart: it has been linked to rare cases of human transmission, usually requiring prolonged, close exposure.
That distinction has sharpened concern aboard the Hondius. Early assumptions held that any outbreak would likely stem from environmental exposure, perhaps through contact with rodents during shore excursions. But confirmation of the Andes strain has forced a reassessment. Health authorities now consider it plausible that transmission could have occurred between passengers, especially in the confined quarters of a ship. The response has echoed familiar pandemic-era measures: isolation of suspected cases, rigorous hygiene practices, and contact tracing. Though the scale remains small, the episode illustrates how even a low-probability transmission pathway can complicate containment strategies.
The origins of the outbreak remain uncertain. Some passengers, including a Dutch couple who later died, had travelled through South America before boarding the ship. That region, particularly parts of Argentina and Chile, is known to harbour the Andes virus in rodent populations. It is conceivable that exposure occurred on land, with symptoms emerging only after departure. The virus’s incubation period—ranging from one to eight weeks—makes such scenarios difficult to unravel. Alternately, exposure may have occurred during the voyage itself, especially given the ship’s itinerary through remote wildlife areas where human contact with infected rodents is more likely.
Symptoms of hantavirus infection vary depending on the strain but can be severe. One form, hantavirus pulmonary syndrome (HPS), begins with flu-like symptoms—fever, fatigue, and muscle aches—before, in some cases, progressing to acute respiratory distress. Mortality rates for HPS can range from 20 per cent to 40 per cent, making it one of the more dangerous viral respiratory illnesses, albeit a rare one. Another form, Haemorrhagic Fever with Renal Syndrome (HFRS), affects the kidneys and can lead to internal bleeding, low blood pressure and acute renal failure. Both conditions require prompt medical intervention, often involving intensive care, oxygen therapy or dialysis.
Despite its severity, hantavirus remains relatively uncommon worldwide. An estimated 150,000 cases of HFRS occur annually, concentrated in parts of Europe and Asia, with China accounting for a substantial share. In the United States, fewer than 1,000 cases have been recorded over three decades. Yet sporadic outbreaks continue to surface, often linked to environmental exposure. In 2025, for instance, the death of Betsy Arakawa, wife of actor Gene Hackman, was attributed to hantavirus infection contracted in a rodent-infested outbuilding. Such incidents underscore the virus’s persistence in both rural and peri-urban settings.
In India, hantaviruses occupy an intriguing niche. The first known isolate, the Thottapalayam virus, was identified in 1964 from a shrew captured in Vellore, indicating that South Asia hosts its own variants. Subsequent studies have detected hantavirus antibodies among high-risk groups, including tribal rodent trappers and warehouse workers, suggesting prior exposure. Research has also confirmed the presence of infected small mammals—bandicoot rats, black rats and house mice—particularly in southern regions. Yet documented human cases remain rare, often presenting as undifferentiated febrile illness or kidney-related complications.
This apparent rarity may be misleading. Clinicians note that hantavirus infections can resemble more common diseases such as dengue, leptospirosis or scrub typhus, leading to underdiagnosis. In settings where laboratory testing is limited, cases may go unrecognised altogether. The overlap in symptoms complicates surveillance efforts and may obscure the true burden of disease. While large-scale outbreaks have not been recorded in India, the ecological conditions—dense populations, variable sanitation, and abundant rodent hosts—suggest that the virus has ample opportunity to circulate at low levels.
The risk factors are well understood. Hantaviruses thrive where rodents and humans intersect, particularly in environments with poor sanitation or inadequate waste management. Activities that disturb contaminated dust—such as cleaning storage spaces, handling grain, or entering abandoned buildings—can aerosolise viral particles. In rural and semi-urban areas, such exposure is common. Yet awareness remains limited, and preventive measures are often overlooked. Even in countries where the virus is better studied, public understanding tends to lag behind scientific knowledge.
Treatment options are similarly constrained. There is no specific antiviral therapy for hantavirus infection, and no widely available vaccine. Care is largely supportive, focusing on symptom management and prevention of complications. Early recognition can improve outcomes, particularly in cases of HPS where timely respiratory support may be life-saving. Some vaccines exist in China and South Korea for region-specific strains, but their use is limited and not globally standardised. Experimental therapies are under investigation, though none have yet transformed clinical practice.
Against this backdrop, the Hondius outbreak appears less as an anomaly than as a convergence of known risks. A mobile population, exposure in endemic regions, and a pathogen with a long incubation period create conditions ripe for delayed detection. The added wrinkle of potential human-to-human transmission, however rare, complicates the picture. It raises questions about how such pathogens should be managed in confined settings and whether existing protocols are sufficient.
For now, health authorities stress that the broader risk remains low. There is no evidence of spread beyond the ship, and hantaviruses do not possess the ease of transmission seen in more familiar respiratory viruses. Yet the episode serves as a reminder that global health is shaped not only by high-profile pandemics but also by a constellation of lesser-known threats. These pathogens may emerge sporadically, often in remote or overlooked settings, but they still demand vigilance.
In an era of rapid travel, the boundaries between local and global health risks are increasingly porous. The story of hantavirus—from its discovery in a South Korean river valley to its appearance on a cruise ship in the Atlantic—illustrates how pathogens can traverse continents with ease. It also highlights the importance of surveillance, research and public awareness in managing diseases that, while rare, carry significant consequences when they do appear.
-30-
Copyright©Madras Courier, All Rights Reserved. You may share using our article tools. Please don't cut articles from madrascourier.com and redistribute by email, post to the web, mobile phone or social media.Please send in your feed back and comments to [email protected]